From pelvic mesh to medication: The latest on bladder control treatments

When we think about the most prevalent health issues affecting Australians, conditions like cancer, arthritis and heart disease often come to mind. But there’s another issue affecting millions Australians: bladder leakage.
There are 4.2 million Australians living with bladder leakage and many of them are suffering in silence. While bladder leakage and incontinence isn’t a topic that many people feel comfortable talking about openly, there are thankfully effective treatments that can reduce the severity of leakage and even put an end to it once and for all.
Stress and urge incontinence are the two most common types of bladder leakage. Stress incontinence refers to leakage triggered by a cough, sneeze or a strain, while urge incontinence is where people experience a sudden and uncontrollable urge to urinate.
“They’re quite different. As a result, there’s a whole bunch of different treatments for each,” Dr Tom Jarvis, Urological Surgeon at Sydney’s Prince of Wales Hospital, tells Starts at 60.
More treatments for the condition have become available in recent years, with a recent market research report revealing the pharmacy industry intends to increase its focus on treatments for overactive bladders over the next four years.
Bladder leakage is often a symptom of other serious health issues and with rising instances of chronic illnesses around the world, continence issues have become more prevalent, driving demand for more medicinal and non-pharmacological options to treat the issue.
Medication
In Australia, two main groups of medication are offered to treat urge incontinence, but there’s currently no medication option available for stress incontinence. Those living with urge incontinence may be prescribed anticholinergics, which work by blocking a receptor on the bladder that causes the bladder to spasm. Another common medication is Beta 3 agonists, which stimulate a receptor that causes the bladder to relax.
“They work in very different ways, but they essentially do the same thing for the bladder,” Jarvis explains.
Medication is typically prescribed as part of a wider treatment plan to combat bladder leakage.
“We normally suggest that patients have tried all the other measures and continue to try all the other measures while they’re on medication because we know the medications work better when they do that,” Jarvis says.

Pelvic floor exercises
Pelvic floor exercises are strongly encouraged for anyone with stress or urge incontinence – even for patients who use medication or have undergone surgical treatment.
Women can strengthen the pelvic floor muscles by imagining they’re holding the flow of urine, holding in wind and trying to squeeze, pull up and hold the muscles in that area. It’s similar for men, who will see their scrotum lift and penis retract when they do the same. Continence experts recommend completing these exercises three times a day.
“We know that even if a person does need medications or other treatment that having a strong pelvic floor will make the medication and other treatments more effective,” Jarvis says.
Read more: Pelvic floor exercises to assist with incontinence
Diet
While some people are tempted to limit fluid intake to prevent leakage, doing so can actually cause further problems.
“That can sometimes lead to more leaking because the urine is really concentrated and irritates the bladder wall more,” Jarvis explains.
Caffeine found in coffee, tea and energy drinks can irritate the bladder and should be replaced with water or decaffeinated beverages where possible. A daily caffeine limit of 100mg is advised for those living with bladder leakage and continence issues, which still allows people to consume one cup of coffee per day.
Carbonated drinks – including mineral water – should also be avoided when possible as the carbon dioxide in the drink makes urine more acidic and therefore more prone to irritating the bladder.
Some people may also find that spicy foods and alcohol upset the bladder and cause more leakage.

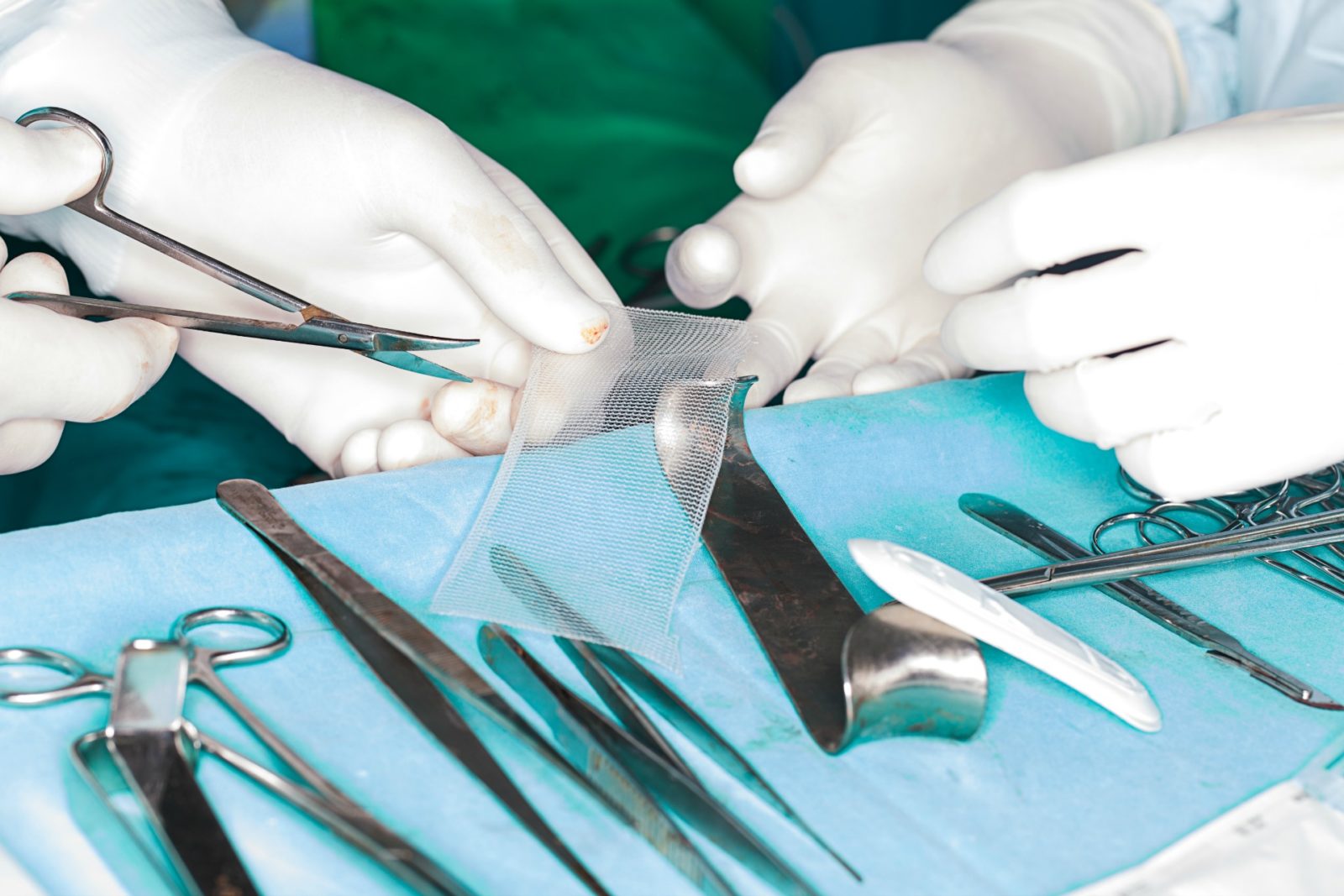
The Therapeutic Goods Administration banned many pelvic mesh devices in 2017 after thousands of women who had been fitted with the mesh to treat pelvic organ prolapse complained the device caused debilitating pain. However, some types of the mesh, such as mid-urethral slings, are still considered safe to treat stress incontinence.
“We still use mesh for stress incontinence in some occasions and that’s where we put a sling around the water pipe [urethra] to hold it when women cough and sneeze and it stops them from leaking,” Jarvis says.
The operation is usually offered when other treatments don’t work.
“We don’t want people jumping straight into surgical options,” Jarvis says. “Some women don’t have any other choice. They’re really upset, really unhappy and have a terrible quality of life due to their leakage and they need a solution.”
Other surgeries
There are different types of surgery available depending on the type of incontinence a person is living with.
For stress incontinence, fascial slings can be constructed from a patient’s own tissue to lift the urethra and bladder to prevent leaks related to stress incontinence. Injections that add bulk to the urethra are also available, while surgeries such as a colposuspension can also lift the urethra to prevent leaks.
Where medication fails in cases of urge incontinence, three main surgeries are offered.
The first is Botox injections, which relax nerves in the bladder to prevent spasms and leakage and help reduce the feeling of having to urinate suddenly. Another options is sacral neuromodulation, where a pacemaker is inserted under the skin to tickle the nerve that supplies the bladder. For others, percutaneous tibial nerve stimulation is best. This treatment sees a small acupuncture needle inserted in the lower leg to stimulate a nerve that causes the bladder to relax.
“The trick in all this is to tailor the treatment to the patient. It’s definitely not a one-size-fits-all situation,” Jarvis says. “It’s about helping the patients know what the treatment options are and choosing one that might best suit them.”
Read more: Don’t let bladder issues interfere with a happy life









 Proudly Australian owned and operated
Proudly Australian owned and operated