Tips to help soothe eczema flare ups

Winter is well and truly here, and while its arrival means cosy blankets and warm drinks, it also brings a not-so-welcome guest: the heightened risk of itchy skin and eczema flare-ups.
The combination of colder temperatures and drier air can wreak havoc on our skin, leaving us desperately searching for solutions to maintain our health and comfort.
With that in mind, Starts at 60 spoke to Caroline Robertson, a Naturopath from Flannerys Mona Vale, to better understand ways to manage your skin during winter.

While it’s not contagious and there’s no exact known cause, eczema is a recurring, non-infectious, inflammatory skin condition that’s caused by a number of internal and external triggers. This results in the skin becoming dry, itchy, scaly and can even cause it to crack and bleed in extreme cases.
“There are many underlying causes of this inflammation,” Robertson said.
“It’s very individualised what triggers a person’s eczema.”
People with a family history of eczema, asthma and even hay fever are more likely to experience it and a dermatologist will formally diagnose eczema through skin examinations and by analysing a person’s medical history. There’s no single test to diagnose eczema and it’s usually a process of eliminating other skin conditions.
Treatments such as corticosteroids, antihistamines, antibiotics and probiotics can be prescribed or purchased over the counter, but it’s important to talk to a medical professional about the best option and possible side effects before use. Equally, other natural treatments are available but should be discussed with a health professional.
Keeping the skin moist and hydrated with oils and creams is the most effective way to keep symptoms at bay. Robertson describes winter as “a danger time” for eczema and that moisturising is vital to prevent skin from cracking and bleeding. When this happens, the skin becomes more susceptible to germs and infections.
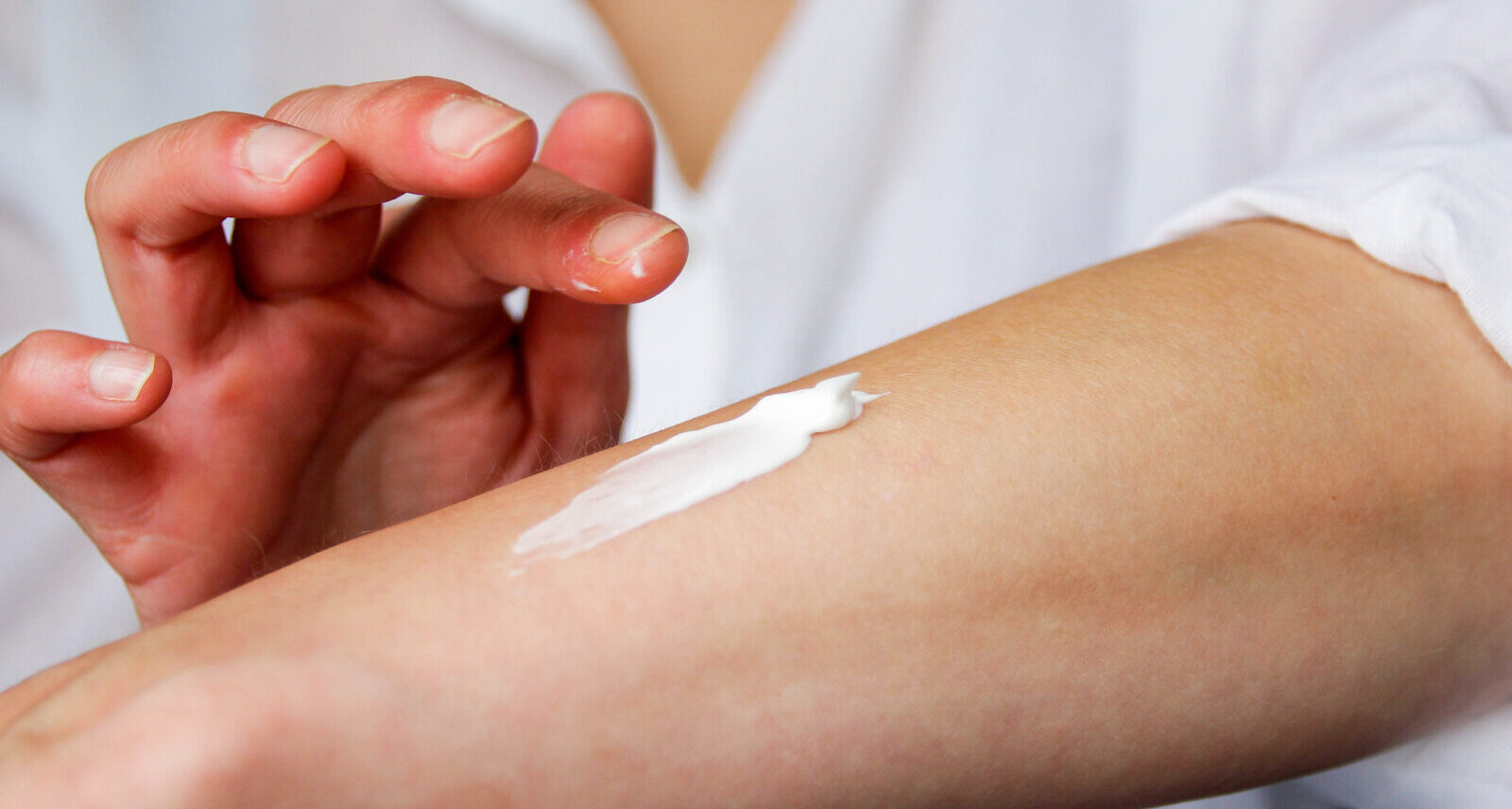
“The kind of oils that tend to help eczema are shea butter, jojoba oil, rosehip oil, sesame oil,” Robertson says.
These ingredients are anti-inflammatory, hydrating and prevent itching. Vitamin E oil is more expensive but according to a study published in the Journal of Research in Medical Sciences, can improve symptoms and quality of life.
Diet can cause eczema but because certain foods impact individuals differently, it can be a process of elimination to determine what’s actually triggering a flare-up.
“Sometimes it’s a matter of getting an allergy test or doing the food tolerance test where you just delete that from your diet and reintroduce it slowly and see if it re-aggravates eczema,” Robertson says.
The most common food irritants include alcohol, dairy, sugar, yeast, gluten, acidic foods and preservatives. Consuming alkaline foods (fruits, nuts, legumes and vegetables) and whole food diets (high in grains, beans, legumes, nuts and seeds) can ease symptoms in many cases and dieticians will be able to offer individualised diet assistance.

Internal hydration is also important and Robertson says keeping refreshed with water and herbal teas instead of coffee or caffeine can improve side effects.
Elsewhere, elements in the environment can trigger eczema for some and the cooler and dry conditions of winter can trigger itchy skin and flare-ups. Heaters or warm showers can also cause skin reactions, while flare-ups may also be caused by allergens, fragrances and soaps.
Opt for fragrance-free creams, lotions and washes, reduce heating and shower temperatures and talk to a health professional if you think clothing, pets, pollen or other common triggers are impacting skin health.
“Some people are lucky and it clears up for life and others are unlucky and it keeps poking its little head out occasionally,” Robertson says of eczema.
“Just by avoiding triggers, some people at least minimise their outbreaks.”
This article was originally published on May 16, 2019 and has been updated on June 9 2023.
IMPORTANT LEGAL INFO This article is of a general nature and FYI only, because it doesn’t take into account your personal health requirements or existing medical conditions. That means it’s not personalised health advice and shouldn’t be relied upon as if it is. Before making a health-related decision, you should work out if the info is appropriate for your situation and get professional medical advice.









 Proudly Australian owned and operated
Proudly Australian owned and operated