Chronic Obstructive Pulmonary Disease (COPD) can be a difficult condition to live with and while flare-ups can cause shortness of breath, a repetitive cough, chest infections and other symptoms, many people use antibiotics as a way of keeping their symptoms at bay.
However, experts now believe the condition – which is an umbrella term given to a series of chronic lung diseases that impact the lungs and airways – may not always need to be managed with antibiotics and found that a simple finger-prick blood test could reduce unnecessary antibiotic use in COPD patients.
Researchers from Cardiff University, the University of Oxford and King’s College London in the United Kingdom demonstrated that using a C-reactive protein (CRP) finger-prick blood test resulted in 20 per cent fewer people using antibiotics for their COPD flare-ups. The study, published in the New England Journal of Medicine, also found the reduction in antibiotic use didn’t have a negative impact on patients’ recovery in the first two weeks after their consultation with a health professional.
In addition, it didn’t impact their well-being or use of health care services in the six months following their initial consultation, with researchers claiming that safely reducing use of antibiotics in this way could help in the battle against antibiotic resistance. Three in four people who experience a COPD flare-up are currently prescribed antibiotics, but the latest study says two thirds of the flare-ups aren’t the result of bacterial infections, meaning antibiotics aren’t likely to benefit these patients.
“Governments, commissioners, clinicians and patients living with COPD around the world are urgently seeking tools to help them know when it is safe to withhold antibiotics and focus on treating flare-ups with other treatments,” researcher Nick Francis said in a statement.
“This is a patient population that are often considered to be at high risk from not receiving antibiotics, but we were able to achieve a reduction in antibiotic use that is about twice the magnitude of that achieved by most other antimicrobial stewardship interventions, and demonstrate that this approach was safe.”
Read more: The everyday hazards linked with rise in deadly COPD
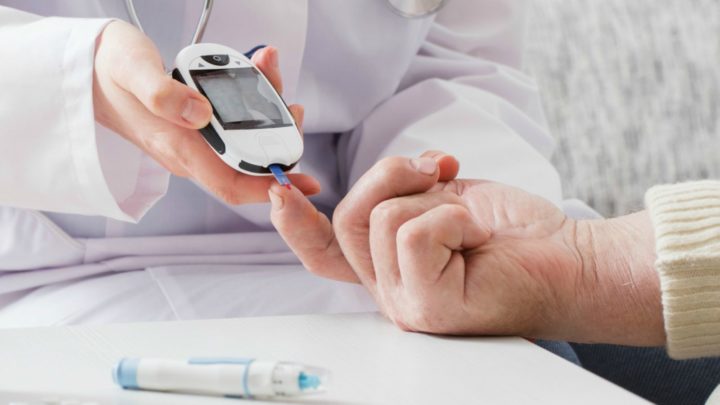
The CRP test measures a marker of inflammation that increases rapidly in the blood in response to serious infections. People experiencing a COPD flare-up and who have lower CRP levels in the blood receive little benefit from antibiotic treatment.
“Acute exacerbations of chronic pulmonary disease account for considerable proportion of unnecessary antibiotic use, but a good solution to the problem in ambulatory care (where most of the antibiotics are prescribed) has not been identified until now,” researcher Chris Butler said. “Ours is the first trial of biomarker guided management of AECOPD in ambulatory care, and has found an effect that should be practice-changing.”
Jonathan Bidmead, who lives with COPD, said the latest study could change the way people living with the condition manage their flare-ups and symptoms.
“As a COPD sufferer, I know that antibiotics are routinely used at the first sign of an exacerbation: this study has shown that doctors can use a simple finger-prick test in a consultation to better identify those instances where antibiotics will probably do no good and may even do some harm,” he said. “This can help us focus on other treatments that may be more helpful for some exacerbations.”
In addition to antibiotics, people may be able to manage symptoms with inhalers, COPD medicines, oxygen therapy and other lifestyle factors, but it’s always important to speak with a health professional about the best treatment options.
Read more: How to stay safe this winter while living with COPD